How are beta cells affected by diabetes?
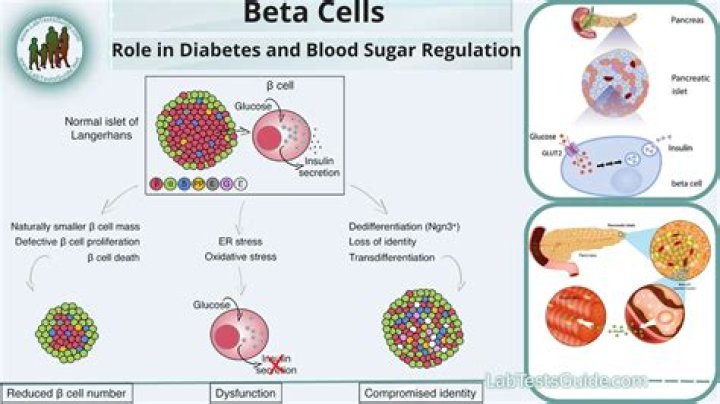
How are beta cells affected by diabetes?
Beta cells are cells in the pancreas that produce and release insulin in response to blood glucose levels. In people with type 2 diabetes, beta cells have to work harder to produce enough insulin to control high blood sugar levels. This can lead to beta cells being unable to work properly to regulate blood sugar.
What are insulin secretory granules?
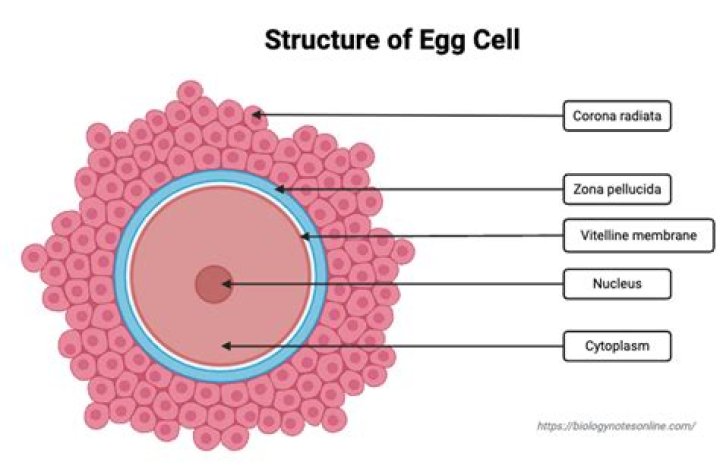
Insulin secretory granules (ISGs) are cytoplasmic organelles of pancreatic β-cells. They are responsible for the storage and secretion of insulin. Furthermore it should give the bases to the comprehension of impaired insulin secretion observed during diabetes.
How is insulin secreted from beta cells?
When the beta cell is appropriately stimulated, insulin is secreted from the cell by exocytosis and diffuses into islet capillary blood. C peptide is also secreted into blood, but has no known biological activity.
Are beta cells damaged in type 2 diabetes?
Pancreatic beta cells that do not produce sufficient insulin in people with type 2 diabetes (T2D) are not permanently damaged during the early stages of the disease and can be restored to normal function through the removal of excess fat in the cells, according to a study entitled “Remission of Type 2 Diabetes for Two …
What causes beta cell damage in type 2 diabetes?
Chronic exposure to elevated levels of glucose and free fatty acids (FFAs) causes β-cell dysfunction and may induce β-cell apoptosis in type 2 diabetes. Exposure to high glucose has dual effects, triggering initially “glucose hypersensitization” and later apoptosis, via different mechanisms.
What happens to beta cells in type 1 diabetes?
With type 1 diabetes, beta cells produce little or no insulin. Without enough insulin, glucose builds up in the bloodstream instead of going into the cells. This buildup of glucose in the blood is called hyperglycemia.
How insulin is secreted?
Insulin is normally secreted by the beta cells (a type of islet cell) of the pancreas. The stimulus for insulin secretion is a HIGH blood glucose…it’s as simple as that! Although there is always a low level of insulin secreted by the pancreas, the amount secreted into the blood increases as the blood glucose rises.
What is insulin granule exocytosis?
Regulated exocytosis is a multistage process involving transport of granules to the plasma membrane, docking of the vesicles with the plasma membrane, and fusion causing release of the contents. Insulin is transported in pancreatic beta cells in large dense core vesicles (LDCV), termed secretory granules.
What does beta cells secrete?
Beta cells secrete insulin, a well-characterized hormone that plays an important role in regulating glucose metabolism.
What is beta cell secretion?
Beta cells (β-cells) are a type of cell found in pancreatic islets that synthesize and secrete insulin and amylin. Beta cells make up 50–70% of the cells in human islets. In patients with Type 1 diabetes, beta-cell mass and function are diminished, leading to insufficient insulin secretion and hyperglycemia.
Do beta cells secrete insulin?
Insulin is secreted by the β-cells of the pancreatic islets of Langerhans in response to elevation of the intracellular Ca2+ concentration ([Ca2+]i). This is produced by an influx of extracellular Ca2+ via voltage-dependent Ca2+ channels, whose activity, in turn, is regulated by the β-cell membrane potential.
What attacks and destroys beta cells of the pancreas?
Pancreatic beta cells are destroyed by T cells of the immune system, precipitating type 1 diabetes (T1D).