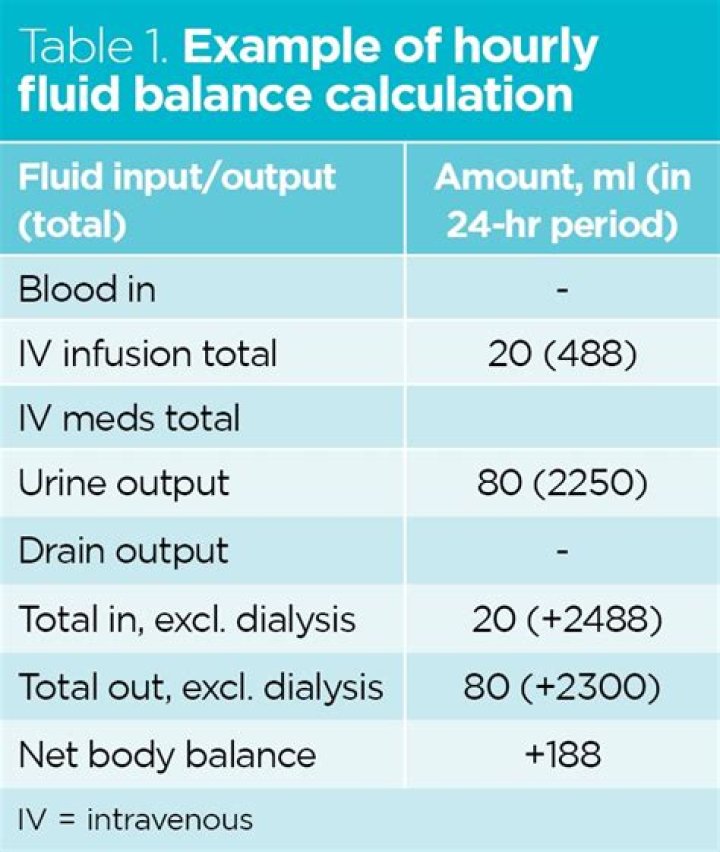
How do you calculate 24 hour fluid balance
100 ml/kg/24-hours = 4 ml/kg/hr for the 1st 10 kg.50 ml/kg/24-hours = 2 ml/kg/hr for the 2nd 10 kg.20 ml/kg/24-hours = 1 ml/kg/hr for the remainder.
How do you calculate ICU fluid balance?
Cumulative fluid balance was calculated as follows: total fluid input minus total fluid output within the first 72 h of ICU stay.
How do you calculate daily fluid maintenance?
- For 0 – 10 kg = weight (kg) x 100 mL/kg/day.
- For 10-20 kg = 1000 mL + [weight (kg) x 50 ml/kg/day]
- For > 20 kg = 1500 mL + [weight (kg) x 20 ml/kg/day]
What is 24-hour fluid balance?
A fluid balance chart is used to document a patient’s fluid input and output within a 24-hour period. This information is used to inform clinical decisions (such as medication and surgical interventions) from medical staff, nurses and dieticians, who all expect accurate figures in exact measurements (Georgiades 2016).How do you calculate fluid deficit?
The first step is to calculate the fluid deficit. This is determined by multiplying the percentage dehydration times the patient’s weight (e.g. 10% dehydration in a 10 kg child: 10% of 10 Kg = 1 kg = 1 liter). Subtract any boluses from this volume (e.g. 1 liter – 400 ml of boluses = 600 ml).
How do you calculate fluid overload?
The degree of fluid overload was expressed as percent fluid overload (%FO), which was calculated by the following formula: [∑ daily (fluid intake (L)-total output (L))/baseline body weight (in kilograms)] x 100. Baseline body weight was obtained from the first available documented weight after visiting the hospital.
What is normal fluid balance?
The core principle of fluid balance is that the amount of water lost from the body must equal the amount of water taken in; for example, in humans, the output (via respiration, perspiration, urination, defecation, and expectoration) must equal the input (via eating and drinking, or by parenteral intake).
What is a normal value for 24 hr urine osmolality and volume?
A 24 hour urine osmolality should average between 500 and 800 mOsm/Kg.How many ml should a person urinate in 24 hours?
Normal Results The normal range for 24-hour urine volume is 800 to 2,000 milliliters per day (with a normal fluid intake of about 2 liters per day). The examples above are common measurements for results of these tests. Normal value ranges may vary slightly among different laboratories.
How can I measure my urine output?To calculate the rate of urine output, divide the volume of urine produced by the number of hours that have elapsed since the bag/chamber was last emptied (e.g. 80ml over 2 hours = 40ml/hour).
Article first time published onHow do you calculate fluid deficit maintenance?
- For children with ≤5% dehydration, replace deficit in the first 24 hours.
- For children with >5% dehydration, replace deficit more slowly.
How do you calculate IV fluid flow rate?
To calculate the drops per minute, the drop factor is needed. The formula for calculating the IV flow rate (drip rate) is total volume (in mL) divided by time (in min), multiplied by the drop factor (in gtts/mL), which equals the IV flow rate in gtts/min.
How do you calculate fluid deficit in adults?
There is no formula to accurately estimate fluid deficit unless the amount of weight loss is known. Clinical indicators such as blood pressure, skin turgor, mental status, and urine output are used to estimate the volume lost. Replacement therapy depends on the extent of dehydration.
How do you measure intake and output?
- 30ml. = oz.
- 2 oz. = ml.
- 2 (8oz.) cups of coffee = ml.
- 1 (6 oz.) bowl of soup = ml.
- 3 (8 oz.) …
- 2 (4 oz.) …
- 2 (4 oz.) …
- 100% (6 oz.)
What is intake and output chart?
The intake and output chart is a tool used for the purpose of documenting and sharing information regarding the following: Whatever is taken by the patient especially fluids either via the gastrointestinal tract (entrally) or through the intravenous route (parenterally) Whatever is excreted or removed from the patient.
How do you calculate fluid deficit in DKA?
Calculations should be double checked before prescribing fluid and insulin. Fluid rate equals (2 x daily maintenance + deficit) ÷ 48.
How do you calculate IV fluids for adults?
- 100 ml/kg/24-hours = 4 ml/kg/hr for the 1st 10 kg.
- 50 ml/kg/24-hours = 2 ml/kg/hr for the 2nd 10 kg.
- 20 ml/kg/24-hours = 1 ml/kg/hr for the remainder.
How do you calculate IV fluids in a neonate?
Calculate routine maintenance IV fluid rates for term neonates according to their age, using the following as a guide: From birth to day 1: 50–60 ml/kg/day. Day 2: 70–80 ml/kg/day. Day 3: 80–100 ml/kg/day.
How is urine output calculated in nursing?
Normal urine output is 1-2 ml/kg/hr. To determine the urine output of your patient, you need to know their weight, the amount of urine produced, and the amount of time it took them to produce that urine. Urine output should be measured at least every four hours if possible.
Which are examples of preformed water?
- Water in an apple.
- Water in a baked potato and steak dinner.
- Water in a glass of milk.
What is the normal urine output per hour?
Normal urine output is defined as 1.5 to 2 mL/kg per hour …
What is positive and negative fluid balance?
The person is said to be in negative fluid balance if his output is greater than his intake. Conversely, a positive fluid balance occurs when intake is greater than output.
Should your intake and output be equal?
Intake & Output. The process involves recording all the fluid that goes into the patient and the fluid that leaves the body. Remember in normal conditions the intake should equal output in 24 hours.
What is the ICD 10 code for fluid overload?
E87. 70 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is fluid volume excess?
Fluid Volume Excess (FVE), or hypervolemia, refers to an isotonic expansion of the ECF due to an increase in total body sodium content and an increase in total body water.
What is the ICD 10 code for volume overload?
E87. 70 – Fluid overload, unspecified. ICD-10-CM.
How often should you pee in 24 hours?
It’s considered normal to have to urinate about six to eight times in a 24-hour period. If you’re going more often than that, it could simply mean that you may be drinking too much fluid or consuming too much caffeine, which is a diuretic and flushes liquids out of the body.
What is considered low urine output?
Oliguria is considered to be a urinary output of less than 400 milliliters, which is less than about 13.5 ounces over the course of 24 hours. The absence of urine is known as anuria. Less than 50 milliliters or less than about 1.7 ounces of urine in a 24-hour period is considered to be anuria.
How many ounces does a person pee?
AgeAverage bladder sizeTime to fill bladderChild (4–12 years)7–14 ounces2–4 hoursAdult16–24 ounces8–9 hours (2 ounces per hour)
What is normal fluid output?
The normal range of urine output is 800 to 2,000 milliliters per day if you have a normal fluid intake of about 2 liters per day. However, different laboratories may use slightly different values. Your doctor will explain what your particular numbers mean.
What is the normal urine output per day nursing?
Normal Results The normal range for 24-hour urine volume is 800 to 2,000 milliliters per day (with a normal fluid intake of about 2 liters per day).