Is Enterobacter aerogenes lactose positive?
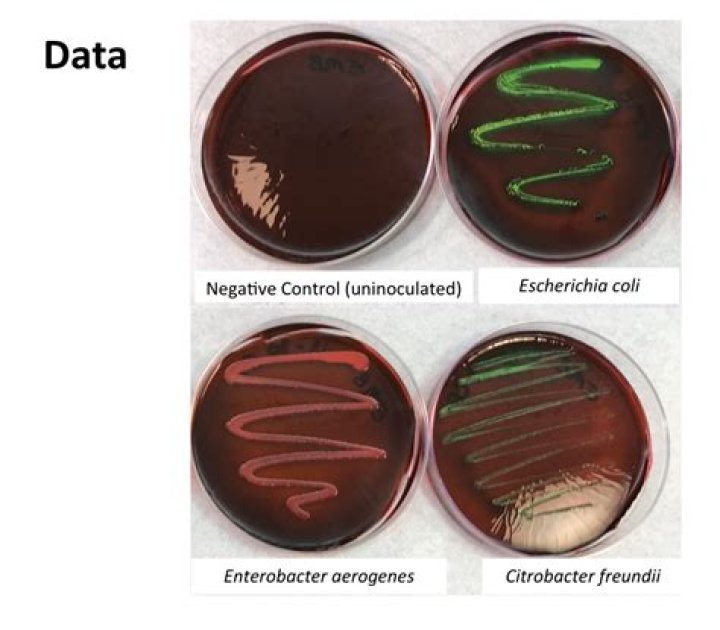
Is Enterobacter aerogenes lactose positive?
here. These bacteria ferment lactose, are motile, and form mucoid colonies. Enterobacter strains commonly arise from the endogenous intestinal flora of hospitalized patients but can occur in common source outbreaks or are spread from patient to patient.
Is Enterobacter aerogenes positive or negative?
Klebsiella aerogenes, previously known as Enterobacter aerogenes, is a Gram-negative, oxidase negative, catalase positive, citrate positive, indole negative, rod-shaped bacterium. The bacterium is approximately 1-3 microns in length, and is capable of motility via peritrichous flagella.
Does Enterobacter aerogenes have amylase?
coli isolates demonstrated catalase and amylase and ß-Lactamase activity, while 77.4% and 67.7%, of Enterobacter aerogenes isolates exhibited catalase, amylase and lipase activity, respectively. Maximum 82.1% and 78.5 of the Pseudomonas aeruginosa showed lipase and catalase activity respectively.
Which test is positive for Enterobacter?
Enterobacter usually have a negative methyl-red test, a positive Voges-Proskauer test, can use citrate as a carbon source, can grow in Moller’s KCN medium at 30 °C, and are ornithine positive, although ‘Enterobacter agglomerans complex’ is ornithine decarboxylase negative (Abbott, 2007).
Is Enterobacter the same as E coli?
Enterobacteriaceae are Gram-negative bacteria of a large family that includes Escherichia coli, Klebsiella, Salmonella, Shigella and Yersinia pestis.
Does Enterobacter aerogenes require isolation?
Enterobacter aerogenes is isolated as human clinical specimens from respiratory, urinary, blood, or gastrointestinal tract (Langley et al., 2001).
How can you tell the difference between E coli and Enterobacter aerogenes?
E. coli is indole-positive; Enterobacter aerogenes is indole- negative. Glucose is the major substrate oxidized by enteric bacteria for energy production. The ability to produce a large amount of acid is used to differentiate E.
What disease does Enterobacter aerogenes cause?
Enterobacter aerogenes can cause gastrointestinal infections, urinary tract infections (UTIs), skin and soft tissue infections, respiratory infections, and adult meningitis.
How do you treat Enterobacter aerogenes?
The antimicrobials most commonly indicated in Enterobacter infections include carbapenems, fourth-generation cephalosporins, aminoglycosides, fluoroquinolones, and TMP-SMZ. Carbapenems continue to have the best activity against E cloacae, E aerogenes, and other Enterobacter species.
Are Enterobacteriaceae glucose positive or negative?
Human Pathogenic Enterobacteriaceae Nearly all are facultative anaerobes. They ferment glucose, reduce nitrates to nitrites, and are oxidase negative.
How do you test for Enterobacter?
The most important test to document Enterobacter infections is culture. Direct Gram staining of the specimen is also very useful because it allows rapid diagnosis of an infection caused by gram-negative bacilli and helps in the selection of antibiotics with known activity against most of these bacteria.
How do you get Enterobacter infection?
According to the National Nosocomial Infections Surveillance System, Enterobacter is a common pathogen discovered from respiratory sputum, surgical wounds, and blood found in isolates from intensive care units (ICU).
Is the Enterobacter aerogenes a Gram negative bacterium?
This confirmed that Enterobacter aerogenes was the gram-negative bacterium. A Methyl Red test was also performed to confirm this answer. The bacterial growth was stirred into the MR-VP and protein broth in order to determine if acid could be produced as a result of glucose fermentation.
How is Enterobacter aerogenes related to Klebsiella cloacae?
In actuality, research shows that “E. aerogenes is more related to Klebsiella aerogenes (47-64%) than it is to E. cloacae (44%) (9). Different species of Enterobacter like E. cloacae are known to be found on a number of seeds and plants while E. sakazakii is commonly seen in infants who were given infant milk-based powder formulas (9).
How is methyl red test performed on Enterobacter aerogenes?
A Methyl Red test was also performed on the gram-negative bacteria to determine whether or not the bacterium produced acid after fermenting glucose. A flame sterilized inoculating loop with bacterial growth on it was stirred around the tube of the protein and glucose MR-VP medium and incubated at 35°C for forty-eight hours.
Why is Enterobacter classified as an ESKAPE pathogen?
Because of the germ’s emerging multi-drug resistance and prevalence in nosocomial infections, it has been grouped as an ESKAPE pathogen ( Enterococcus, Stapylococcus, Klebsiella, Acinetobacter, Pseudomonas, and Enterobacter species).