Is Group B Strep sensitive to clindamycin?
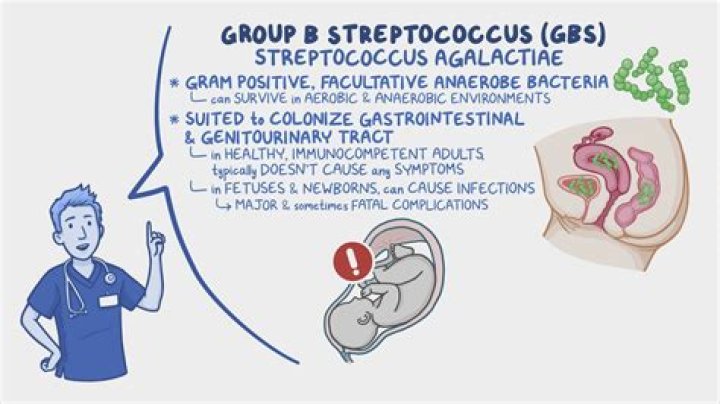
Is Group B Strep sensitive to clindamycin?
Erythromycin resistance was present in 22% of GBS isolates, and these isolates were constitutively resistant, inducibly resistant, or sensitive to clindamycin.
Does clindamycin cover beta hemolytic strep?
Clindamycin has been increasingly used as an agent capable of treating both CA-MRSA and beta-hemolytic streptococci. The appeal of clindamycin for SSTI includes its activity against many streptococci and S.
What does inducible clindamycin resistance mean?
In MLS-B bacterial strains, erythromycin induces production of a methylase enzyme, which allows clindamycin resistance to be expressed. Inducible clindamycin resistance is determined by means of an antibiotic disk diffusion test, called the D-test, which requires overnight incubation of the organism being tested.
Does clindamycin cover streptococcus?
Clindamycin is a lincosamide antibiotic that has been approved by the US Food and Drug Administration for the treatment of anaerobic, streptococcal, and staphylococcal infections.
Is resistance to clindamycin common?
Local outbreaks of clindamycin resistance have been noted in the United States and in Europe. The susceptibility of Bacteroides in the United States in 1983 from a multi-center study reveals a 5% incidence of resistance in B.
Can bacteria become resistant to clindamycin?
Antimicrobial Activity Most aerobic gram-negative bacteria, such as Pseudomonas spp and H. influenzae, are inherently resistant to clindamycin because of poor permeability of the cellular outer envelope to the drug. An exception is Capnocytophaga canimorsus, which is highly susceptible to clindamycin.
How common is clindamycin resistance?
Erythromycin and clindamycin resistance was seen in 54.4% (147/270) and 41.8% (113/270) isolates respectively. Resistance to erythromycin and clindamycin were higher in MRSA as compared to MSSA (erythromycin-resistance: 88.2% Vs 39.1% and clindamycin-resistance: 79.4% Vs 41.8%).
What bacteria is sensitive to clindamycin?
Susceptible bacteria Anaerobic, Gram-negative rod-shaped bacteria, including some Bacteroides, Fusobacterium, and Prevotella, although resistance is increasing in Bacteroides fragilis.
What bacteria are susceptible to clindamycin?
Clindamycin is indicated in the treatment of serious infections caused by susceptible anaerobic bacteria. Clindamycin is also indicated in the treatment of serious infections due to susceptible strains of streptococci, pneumococci, and staphylococci.
Does clindamycin resistance go away?
When we use clindamycin alone topically, even in acne, it is more likely to cause bacterial resistance. However, when we combine clindamycin with benzoyl peroxide, the chance of resistance decreases significantly.