What is a major complication of TPN?
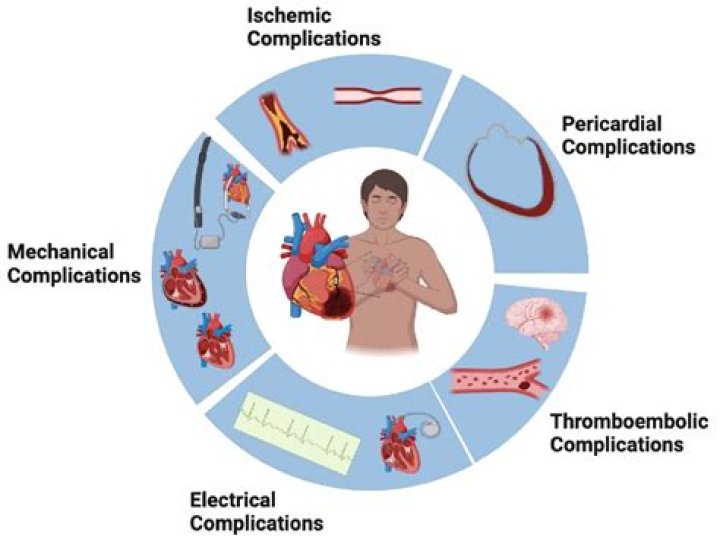
What is a major complication of TPN?
Possible complications associated with TPN include: Dehydration and electrolyte Imbalances. Thrombosis (blood clots) Hyperglycemia (high blood sugars) Hypoglycemia (low blood sugars)
What is the most common complication of parenteral nutrition?
Fatty liver, non-alcoholic fatty liver disease, intrahepatic cholestasis, cholecystitis and cholelithiasis may occur with PN [36], [37]. Fatty liver is the most common complication, whereas intrahepatic cholestasis or hepatitis are less frequent.
What is the most frequently seen serious complication of TPN therapy?
The most common complications associated with TPN is central line infection. Other common complications include abnormal glucose levels and liver dysfunction. TPN use can lead to hyperglycemia, and stopping suddenly can cause hypoglycemia.
What should I monitor during TPN?
Weight, complete blood count, electrolytes, and blood urea nitrogen should be monitored often (eg, daily for inpatients). Plasma glucose should be monitored every 6 hours until patients and glucose levels become stable. Fluid intake and output should be monitored continuously.
What is an example of metabolic complication that can occur with parenteral nutrition support?
The metabolic complications associated with PN in adult patients include hypergly- cemia, hypoglycemia, hyperlipidemia, hy- percapnia, refeeding syndrome, acid–base disturbances, liver complications, manga- nese toxicity, and metabolic bone disease.
What electrolyte imbalances can TPN cause?
TPN Electrolytes (multiple electrolyte additive) is contraindicated in pathological conditions where additives of potassium, sodium, calcium, magnesium or chloride could be clinically deleterious, e.g., anuria, hyperkalemia, heart block or myocardial damage and severe edema due to cardiovascular, renal or hepatic …
Does TPN damage the liver?
One of the major causes of morbidity and mortality in patients receiving long-term total parenteral nutrition (TPN) is liver disease. Early on, there is steatosis, which can evolve to steatohepatitis and eventually to cholestasis of varying severity.
Why does TPN cause cholestasis?
The high prevalence of TPN-associated cholestasis in premature infants is attributed to the relative immaturity of the hepatic canalicular transporters mediating bile secretion. Premature neonates have a decreased bile acid pool and impaired hepatic mitochondrial function.
When is TPN contraindicated?
According to Maudar (2017), TPN is generally contraindicated in the following conditions: Infants with less than 8 cm of the small bowel. Irreversibly decerebrate patients. Patients with critical cardiovascular instability or metabolic instabilities.
Can TPN affect kidneys?
We describe a profound decrease in renal function associated with long-term TPN, most of which is largely unexplained.